Age-related vision changes can arrive quietly first as extra glare while driving at night, then as the sense that colors look muted or fine print seems to “swim” on the page. Because these shifts often build over years, many people normalize them and delay an eye evaluation. Yet the underlying causes vary widely, and today’s treatment options are far broader than most patients realize. From earlier detection to more personalized procedures, modern care focuses on restoring function while protecting long-term eye health.
Why does eyesight change with time?
As we get older, the eye’s natural lens can stiffen, the vitreous gel may shift, and the retina can become more sensitive to stress. Tear production may also decrease, causing occasional blurred vision or fluctuating clarity that can be confusing. Conditions like cataracts, glaucoma, macular degeneration, and diabetic eye disease often overlap, so a personalized approach is essential. Visiting a cataract hospital in Vadodara can help ensure a thorough evaluation and proper treatment, combining expert diagnostics with safe, effective care.
Earlier diagnosis through smarter screening
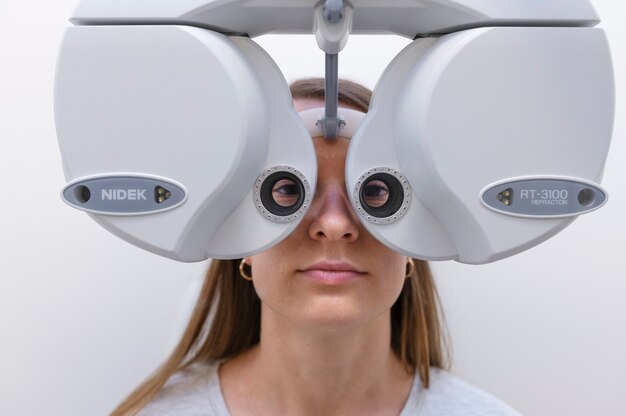
Modern screening does more than read an eye chart. High-resolution imaging can map subtle structural changes long before noticeable vision loss occurs. Optical coherence tomography helps clinicians “see” layers of the retina and optic nerve, supporting earlier intervention for macular degeneration and glaucoma. Widefield retinal photos reveal peripheral abnormalities that were once easy to miss in a routine exam. Even simple improvements like better contrast testing or glare evaluation can reveal functional limitations that traditional testing overlooks. These tools make it easier to track progression over time, so treatment can be timed for maximum benefit rather than waiting until daily life is disrupted.
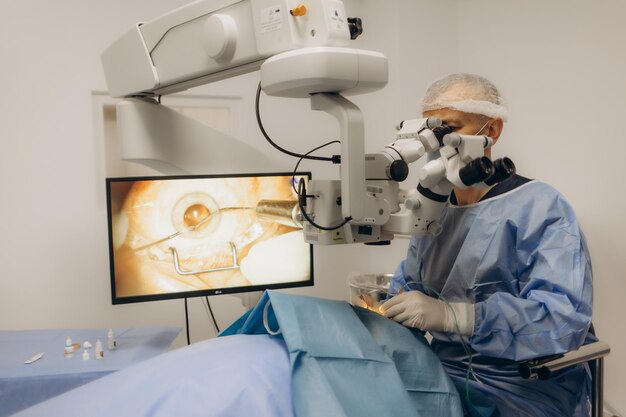
Lens-based solutions for clouding and focusing issues
When the natural lens becomes cloudy or less flexible, vision can dim, blur, and scatter light. Modern procedures are designed to be precise, customized, and quick to recover from. Detailed measurements guide lens selection, and contemporary implant options can address a wider range of focusing needs than standard lenses. Some approaches aim to reduce dependence on glasses for distance or near tasks, though suitability depends on eye health, lifestyle, and tolerance for trade-offs such as halos. The best outcomes come from matching the technique and lens design to the patient’s visual priorities, rather than choosing the most “premium” option by default.
Retinal therapies that protect central vision
For many older adults, the greatest fear is losing the ability to recognize faces or read functions tied to central vision. Treatments for retinal conditions have advanced dramatically, particularly for certain forms of macular degeneration and diabetic macular swelling. Targeted injections can slow harmful blood vessel growth and reduce fluid, preserving vision that might otherwise decline rapidly. Nutritional supplementation may be recommended for specific risk profiles, and careful monitoring helps detect conversion to more aggressive disease stages. While these therapies don’t restore a youthful retina, they can maintain usable sight for years when started promptly and followed consistently.
Pressure control strategies for optic nerve safety
Glaucoma management has evolved beyond a single pathway of eye drops. Newer medications, refined laser procedures, and minimally invasive surgical options can reduce eye pressure with fewer side effects for selected patients. The emphasis today is on protecting the optic nerve before irreversible field loss occurs. Because glaucoma can progress silently, repeat testing and trend analysis matter as much as any single measurement. Clinicians increasingly personalize targets, deciding what “safe pressure” means based on nerve appearance, corneal factors, age, and how quickly changes appear over time.
Personalized optics and functional rehabilitation
Not every vision problem is solved by surgery or medication alone. Modern care includes better refraction methods, specialty contact lenses for irregular corneas, and filters that reduce glare sensitivity. Low-vision services have also changed: enhanced lighting plans, contrast-boosting tools, electronic magnifiers, and phone-based accessibility features can restore independence. Rehabilitation focuses on the tasks that matter most, reading medication labels, cooking safely, and navigating steps, rather than only improving a single test score. Many patients find that combining medical treatment with functional coaching yields the most meaningful quality-of-life improvement.
Recovery and lifestyle guidance after procedures
Healing is often faster now, but the eye still benefits from thoughtful routines that minimize irritation and infection risk. Patients are commonly advised to avoid rubbing, keep water and dust out of the eye, and follow medication schedules precisely. It can also help to plan for supportive habits such as wearing UV-protective sunglasses outdoors and taking short breaks from screens during early recovery. When people ask for cataract healing tips, the most reliable guidance is usually the simplest: use prescribed drops exactly as directed, protect the eye during sleep if instructed, and report sudden pain, worsening redness, or a quick drop in vision without delay.
Technology-led care pathways and coordinated follow-up
Care delivery itself has modernized. Digital imaging can be compared over time with greater accuracy, and clinics increasingly integrate results into streamlined care plans. Remote check-ins, automated reminders, and shared records can reduce missed follow-ups, which is critical for chronic conditions requiring ongoing monitoring. The phrase advanced eye care is often used to describe this mix of precise diagnostics, evidence-based treatments, and structured follow-up that keeps small problems from becoming permanent losses. For patients, the practical advantage is clarity: fewer unknowns, better expectation-setting, and faster adjustments when a plan isn’t working.
Conclusion
Modern treatment for age-related vision loss is no longer limited to “wait and see” or a single procedure. Today’s approaches combine earlier detection, tailored interventions, and supportive rehabilitation so that patients can maintain independence and confidence. The most important step is timely evaluation, especially when glare, blur, distortion, or fading color begins to interfere with daily routines. With the right plan and consistent monitoring, many people can preserve useful vision well into later life and continue doing the activities that make their days feel full.

